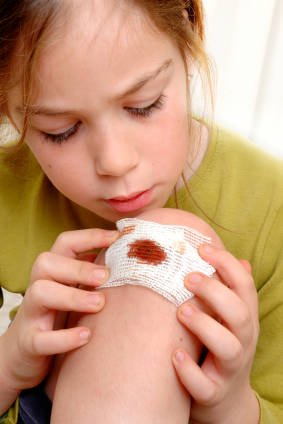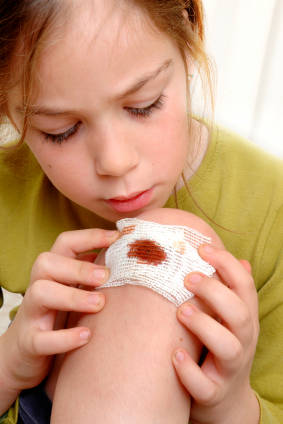
Determining the time and how the wound occurred is a vital assessment because any delay in treatment significantly increases the chances of infection. Using aseptic technique, the clinician visually inspects the wound in order to determine the extent of damage to underlying structures such as sensory, motor and vascular function of the affected part that might indicate any complications.
Management
- Wound Cleaning
The wound is irrigated gently and profusely with normal saline solution to remove any surface dirt embedded in the wound. Devitalize/irreparable tissues and foreign materials are removed because they impede healing and may promote infection. Wounds with deep cuts causing severe bleeding are surgically treated in the emergency department’s minor surgery room wherein the clinician clamps or cauterizes severed blood vessels to achieve hemostasis followed by the application of a nonadherent dressing to protect the wound as well as serving as a splint for immobilization.
Typically, the area around the wound is applied with antibacterial agents such as povidone-iodine (Betadine solution) or hydrogen peroxide. However, these agents should not be allowed to get into deep without thorough rinsing. Betadine solution and hydrogen peroxide are only used for initial cleansing mainly because they injure exposed and healthy tissue resulting in further cellular injury.
- Primary Closure
The decision to suture a wound will depend primarily on the nature of the wound, the time elapsed since the injury, the degree of contamination and the extent of vascular damage. If primary closure is indicated, the individual will undergo minor surgery and suturing under local anesthesia or moderate sedation depending on the physical assessment of the individual.
Wound closure is initiated when the subcutaneous layer is brought loosely with a few sutures to close the gap of the dead space and the subcutaneous layer is then closed. Sutures are normally placed proximal to the wound edge with the skin edges leveled cautiously to promote optimal healing.
- Delayed Primary Closure
Delayed primary closure is usually indicated if the injured tissue has been lost or has a high potential for infection. A thin layer sterile gauze (to make sure proper drainage is maintained and prevent pooling of exudates), covered with an occlusive dressing is often used. If there are no signs of purulent discharges (indicative of infection), the wound may be sutured under local anesthesia. Moreover, antibiotic medication is used in conjunction based on factors such as the manner of injury, time elapsed since injury and the risk of contamination. The site is normally immobilized and elevated to limit the accumulation of fluids in the interstitial spaces of the wound.
Tetanus prophylaxis routinely administered and depending on the condition of the wound as well as the individual’s immunization status will be given either a full course of immunization or just a booster shot.